Select The Four Statements About Plasmodium That Are True.
News Leon
Apr 02, 2025 · 7 min read
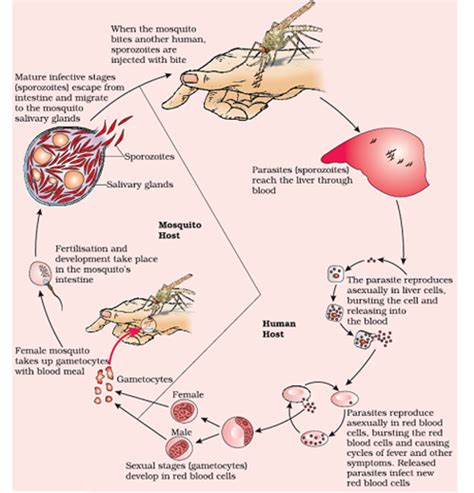
Table of Contents
Four Truths About Plasmodium: Unveiling the Secrets of Malaria's Mastermind
Malaria, a devastating parasitic disease affecting millions globally, is caused by the genus Plasmodium. Understanding this genus is crucial for developing effective prevention and treatment strategies. This article delves into the fascinating world of Plasmodium, highlighting four key truths about its biology, lifecycle, and impact on human health. We'll explore its complex life cycle, its interaction with the human immune system, the challenges in developing effective antimalarial drugs, and the ongoing efforts to eradicate this persistent global health threat.
1. Plasmodium's Complex Life Cycle: A Journey Through Two Hosts
One undeniable truth about Plasmodium is its intricate life cycle, requiring both a mosquito vector and a vertebrate host (primarily humans). This complex process involves multiple stages, each adapted to its specific environment. Understanding this duality is fundamental to comprehending the parasite's transmission and survival.
From Mosquito to Man: The Infectious Stage
The life cycle begins when an infected female Anopheles mosquito, the primary vector, takes a blood meal from a human. During this feed, infectious sporozoites, the motile stage of the parasite, are injected into the bloodstream. These sporozoites quickly travel to the liver, where they undergo asexual multiplication, a process known as exoerythrocytic schizogony. This stage is largely asymptomatic, meaning the infected individual shows no symptoms.
The Erythrocytic Cycle: The Source of Clinical Symptoms
After the liver stage, merozoites—the product of liver schizogony—are released into the bloodstream. These merozoites invade red blood cells (erythrocytes), initiating the erythrocytic cycle. This stage is responsible for the clinical manifestations of malaria, including fever, chills, sweats, and anemia. Within the red blood cells, the merozoites undergo further asexual replication, resulting in the rupture of infected cells and the release of new merozoites, perpetuating the cycle.
Gametocytes: The Bridge to the Mosquito
A crucial aspect of the erythrocytic cycle is the development of gametocytes. These sexual forms of the parasite are essential for the transmission of malaria to the mosquito vector. When a mosquito takes a blood meal from an infected individual, it ingests these gametocytes. In the mosquito's gut, gametocytes undergo fertilization, forming zygotes which develop into ookinetes, and subsequently sporozoites, ready to infect a new human host.
The Significance of Understanding the Life Cycle
The intricacy of the Plasmodium life cycle is not merely a biological curiosity; it holds the key to effective malaria control. Targeting different stages of the cycle, whether in the mosquito vector, the liver, or the red blood cells, forms the basis of diverse antimalarial interventions, including vector control, prophylactic drugs targeting the liver stage, and drugs targeting the erythrocytic stages.
2. Plasmodium's Evasive Strategies: Outsmarting the Immune System
Another critical truth about Plasmodium is its remarkable ability to evade the human immune system. This parasite has evolved sophisticated mechanisms to avoid detection and destruction by immune cells. These evasion strategies contribute significantly to the persistence of malaria infections.
Antigenic Variation: A Constant Game of Hide-and-Seek
Plasmodium exhibits remarkable antigenic variation, meaning it constantly changes its surface proteins. This prevents the immune system from developing long-lasting immunity, as antibodies generated against one variant may not be effective against others. This phenomenon is particularly pronounced in P. falciparum, the most deadly malaria parasite.
Immune Suppression: Weakening the Host's Defenses
Beyond antigenic variation, Plasmodium actively suppresses the host's immune response. The parasite produces molecules that interfere with the function of immune cells, hindering their ability to recognize and eliminate infected red blood cells. This immunosuppression contributes to the severity of malaria and increases susceptibility to other infections.
Sequestration: Hiding in Plain Sight
Certain Plasmodium species, particularly P. falciparum, employ a strategy known as sequestration. Infected red blood cells adhere to the lining of blood vessels, preventing them from reaching the spleen, the primary site of immune cell activity. This allows the parasite to escape immune surveillance and continue its replication cycle undisturbed.
The Immune System's Response: A Complex and Often Ineffective Battle
The human immune system does mount a response against Plasmodium, but its effectiveness varies depending on factors like the parasite species, the host's genetic background, and previous exposure to malaria. While some immunity can develop following repeated infections, it is rarely complete or sterilizing, highlighting the challenge in developing a truly effective malaria vaccine.
3. Antimalarial Drug Resistance: A Growing Threat
The emergence and spread of antimalarial drug resistance represent a significant obstacle in the fight against malaria. The parasite's remarkable adaptability allows it to develop resistance to various drugs, rendering previously effective treatments ineffective.
Mechanisms of Drug Resistance: A Molecular Arms Race
Plasmodium can develop resistance through various mechanisms, including mutations in drug target sites, increased drug efflux (pumping the drug out of the parasite), and altered metabolic pathways. These mechanisms reduce the effectiveness of antimalarial drugs, necessitating the development of new drugs and treatment strategies.
The Impact of Drug Resistance: Increased Mortality and Treatment Failure
Drug resistance leads to treatment failures, prolonged infections, increased morbidity (illness), and mortality (death), particularly in vulnerable populations. This necessitates the constant monitoring of drug resistance patterns and the development of new antimalarial drugs to combat this growing threat.
Combating Drug Resistance: A Multi-pronged Approach
Addressing drug resistance requires a multi-faceted approach. This includes responsible drug use, the development and deployment of new antimalarial drugs with novel mechanisms of action, combination therapies to minimize the risk of resistance development, and accurate diagnosis and surveillance to track the emergence and spread of resistance.
The Ongoing Search for New Antimalarial Drugs: A Vital Necessity
The development of new antimalarial drugs is crucial in maintaining effective malaria control. Researchers are actively exploring novel drug targets and drug classes to combat resistance and improve treatment outcomes. This is an ongoing and essential area of research to overcome the challenge of antimalarial resistance.
4. Eradication Efforts: A Global Challenge
Despite considerable progress, the eradication of malaria remains a formidable challenge. While significant strides have been made in reducing malaria incidence and mortality in many regions, various factors continue to hinder the eradication effort.
Challenges in Malaria Eradication: A Complex Equation
The complex nature of malaria transmission, coupled with factors such as poverty, inadequate healthcare infrastructure, environmental changes, and the emergence of drug resistance, pose substantial obstacles to eradication. These interconnected challenges require a comprehensive and coordinated approach.
The Role of Vector Control: Targeting the Mosquito Vector
Vector control strategies, such as insecticide-treated bed nets, indoor residual spraying, and larvicides, play a vital role in reducing malaria transmission. However, the development of insecticide resistance in mosquitoes poses a significant challenge to the effectiveness of these interventions.
The Importance of Case Management: Prompt and Effective Treatment
Prompt and effective case management, including rapid diagnostic tests and appropriate antimalarial treatment, is crucial in reducing malaria morbidity and mortality. However, access to quality healthcare remains a major challenge in many endemic regions.
The Pursuit of a Malaria Vaccine: A Long-Term Goal
The development of an effective malaria vaccine is a long-term goal that holds the potential to significantly impact malaria control efforts. While several vaccine candidates are under development, none have yet achieved the level of efficacy required for widespread implementation. However, progress continues, and a safe and effective vaccine would represent a substantial step toward eradication.
In conclusion, understanding the complex nature of Plasmodium, from its intricate life cycle and its ability to evade the immune system to the challenges of drug resistance and the ongoing global eradication efforts, is crucial for effectively combating this devastating disease. The ongoing research and collaborative efforts are essential in pushing forward towards a malaria-free world. The future of malaria control depends on continued research, innovation, and collaborative global action.
Latest Posts
Latest Posts
-
Why Are Fleas Hard To Squish
Apr 03, 2025
-
How Many Chromosomes In A Daughter Cell
Apr 03, 2025
-
Why Do Bones Heal Quicker Than Cartilage
Apr 03, 2025
-
Can Magnitude Be Negative In Physics
Apr 03, 2025
-
What Is The Area Of Triangle Rst
Apr 03, 2025
Related Post
Thank you for visiting our website which covers about Select The Four Statements About Plasmodium That Are True. . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
