The Diaphragm Separates The Thoracic Cavity From The
News Leon
Apr 02, 2025 · 7 min read
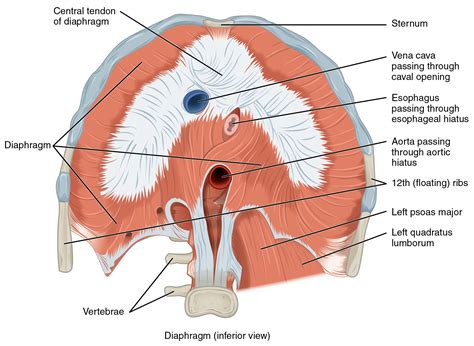
Table of Contents
The Diaphragm: Separating Thoracic and Abdominal Cavities, and its Crucial Role in Respiration
The diaphragm, a remarkable dome-shaped muscle, plays a pivotal role in separating the thoracic cavity (chest cavity) from the abdominal cavity. This seemingly simple anatomical feature is actually a complex and highly efficient structure crucial for breathing, maintaining posture, and supporting various other bodily functions. Understanding its anatomy, physiology, and potential pathologies is essential for appreciating its profound impact on overall health.
Anatomy of the Diaphragm: A Closer Look
The diaphragm is a thin, broad muscle that forms the floor of the thoracic cavity and the roof of the abdominal cavity. Its unique shape resembles an inverted bowl, with its central tendon – a strong, aponeurotic structure – located at the highest point of the dome. This central tendon serves as an attachment point for the muscular fibers that radiate outwards and downwards towards the peripheral attachments.
Attachments and Innervation:
The diaphragm's muscular fibers originate from several key locations:
- Sternal Part: These fibers arise from the posterior surface of the xiphoid process of the sternum (breastbone).
- Costal Part: The largest portion, these fibers originate from the inner surfaces of the lower six ribs and their corresponding costal cartilages.
- Lumbar Part: These fibers arise from two crura (legs) that originate from the lumbar vertebrae (lower back). The right crus is longer and more robust than the left crus. These fibers intertwine to form the median arcuate ligament, medial arcuate ligament and lateral arcuate ligaments. The psoas major muscles and the quadratus lumborum muscles are closely related to the lumbar attachment.
The diaphragm is innervated primarily by the phrenic nerves, which arise from the cervical plexus (C3-C5 spinal nerves). This explains why irritation to these nerves, as can occur in conditions like hiccups or diaphragmatic irritation, can cause referred pain in the neck and shoulder region. Additional sensory innervation is provided by intercostal nerves.
Openings and Passages:
Several important structures pass through the diaphragm, allowing for communication between the thoracic and abdominal cavities. These openings are carefully positioned to prevent herniation or leakage while allowing for the passage of vital structures:
- Caval Opening (Foramen Vena Cavae): Located at the level of T8 vertebra, this opening allows passage for the inferior vena cava (IVC), which returns deoxygenated blood from the lower body to the heart.
- Esophageal Opening (Hiatus): Situated at the level of T10 vertebra, this opening allows passage for the esophagus and the vagus nerves, which control gastrointestinal function. This area is a common site for hiatal hernias.
- Aortic Opening: Located anteriorly to the T12 vertebra, this opening allows passage for the descending aorta, the thoracic duct, and azygos vein.
Physiological Role of the Diaphragm: Breathing and Beyond
The diaphragm's most well-known function is its crucial role in respiration. Its contraction and relaxation drive the mechanics of breathing:
Inhalation: The Diaphragm's Active Role
During inhalation, the diaphragm contracts, causing its dome to flatten and move inferiorly. This downward movement increases the vertical dimension of the thoracic cavity, creating a negative pressure gradient that draws air into the lungs. This process is aided by the external intercostal muscles which lift the ribs and expand the thoracic cage. The increase in volume leads to a decrease in pressure, causing air to rush into the lungs.
Exhalation: A Passive Process Primarily
Exhalation is primarily a passive process. As the diaphragm relaxes, its dome returns to its resting position, decreasing the volume of the thoracic cavity and increasing the pressure inside. This pressure difference forces air out of the lungs. However, during forceful exhalation, such as during exercise or coughing, the internal intercostal muscles and abdominal muscles assist in compressing the thoracic cavity and actively expelling air.
Beyond Respiration: Supporting Other Functions
While its role in respiration is paramount, the diaphragm's functions extend far beyond breathing. Its actions have significant implications for other bodily systems:
- Posture and Stability: The diaphragm's contraction and relaxation contribute to trunk stability and posture. Its strong attachments to the spine and ribs provide support and contribute to the overall biomechanics of the body. Weakness in the diaphragm can lead to poor posture and back pain.
- Venous Return: The diaphragm's action assists in venous return by creating a pressure gradient that facilitates the flow of blood back towards the heart. Its contraction increases abdominal pressure and helps to propel blood towards the superior vena cava.
- Lymphatic Drainage: The diaphragm plays a role in lymphatic drainage, facilitating the movement of lymph fluid throughout the body. Its movement helps to pump lymph towards the thoracic duct.
- Gastrointestinal Function: The diaphragm's interaction with the abdominal viscera influences gastrointestinal motility and function. Its movements assist in the mixing and movement of food through the digestive tract.
- Vocalization: The diaphragm plays a role in vocalization by supporting the lungs and controlling airflow, thus assisting in the production of sound.
Diaphragmatic Pathology: Conditions Affecting Function
Various conditions can affect the diaphragm's structure and function, leading to significant health implications. These conditions may involve:
Diaphragmatic Hernia:
A diaphragmatic hernia occurs when a portion of an abdominal organ protrudes through an opening in the diaphragm. This can lead to symptoms ranging from mild discomfort to severe respiratory distress, depending on the size and location of the hernia. Hiatal hernias, where a portion of the stomach protrudes through the esophageal hiatus, are particularly common.
Diaphragmatic Paralysis:
Diaphragmatic paralysis occurs when the diaphragm's nerve supply (phrenic nerves) is damaged, leading to weakness or complete paralysis of the diaphragm. This can result in shortness of breath, particularly during exertion. Causes can range from trauma to neurological conditions.
Eventration of the Diaphragm:
Eventration of the diaphragm is a condition where the diaphragm is abnormally high and flattened, often due to congenital defects or nerve damage. This reduces its efficiency in respiration.
Diaphragmatic Rupture:
A diaphragmatic rupture is a serious condition usually caused by trauma, such as a car accident or penetrating injury. This can lead to significant respiratory compromise and requires immediate medical attention.
Other Conditions:
Other conditions that can affect the diaphragm include:
- Pleuritis (Pleurisy): Inflammation of the pleura, the membranes surrounding the lungs and lining the chest cavity. This can cause pain that worsens with breathing.
- Pneumonia: Lung infection that can affect breathing and diaphragm function.
- Gastroesophageal Reflux Disease (GERD): Chronic reflux of stomach acid into the esophagus, which can irritate the diaphragm and potentially contribute to hiatal hernia.
Investigating Diaphragmatic Function: Diagnostic Tools
Several diagnostic tools are available to assess diaphragm function and diagnose related conditions. These include:
- Physical Examination: A thorough physical examination can often reveal signs of diaphragmatic dysfunction, including abnormal breath sounds and respiratory distress.
- Chest X-Ray: A chest X-ray can provide an image of the diaphragm, helping to identify structural abnormalities such as hernias or eventration.
- Computed Tomography (CT) Scan: A CT scan provides a more detailed image of the diaphragm and surrounding structures, allowing for a more precise diagnosis.
- Magnetic Resonance Imaging (MRI): An MRI offers high-resolution images of soft tissues, enabling a detailed evaluation of the diaphragm and its associated structures.
- Electromyography (EMG): EMG measures the electrical activity of muscles, providing information about the diaphragm's neuromuscular function and identifying possible nerve damage.
- Phrenic Nerve Conduction Study: This study assesses the integrity of the phrenic nerves.
Treatment Options for Diaphragmatic Conditions: A Range of Approaches
Treatment for diaphragmatic conditions depends on the specific diagnosis and severity of the condition. Options include:
- Conservative Management: For mild conditions, conservative management may be sufficient. This can involve lifestyle modifications such as weight loss, dietary changes, and medication to manage associated symptoms.
- Surgical Repair: Surgical intervention may be necessary for conditions such as diaphragmatic hernias, ruptures, and severe eventration. The specific surgical approach will vary depending on the nature of the condition.
- Respiratory Support: In cases of severe diaphragmatic dysfunction, respiratory support may be required using mechanical ventilation.
Conclusion: The Diaphragm's Unsung Importance
The diaphragm's seemingly simple anatomical structure belies its profound importance in respiratory function, postural stability, and overall health. Its intricate interplay with other bodily systems highlights its crucial role in maintaining homeostasis. Understanding its anatomy, physiology, and potential pathologies provides invaluable insight into the complexities of the human body and the development of effective diagnostic and therapeutic strategies for a range of conditions. Further research continues to uncover the full extent of the diaphragm's influence on health and well-being, emphasizing the need for ongoing investigation and awareness of its significance.
Latest Posts
Latest Posts
-
Which Tissue Is Responsible For Plant Growth
Apr 03, 2025
-
Fill Up The Blanks With The Words Given
Apr 03, 2025
-
Which Of The Following Is True About Tsunamis
Apr 03, 2025
-
Which Of The Following Is Not A Transition Metal
Apr 03, 2025
-
When Air Is Heated What Happens
Apr 03, 2025
Related Post
Thank you for visiting our website which covers about The Diaphragm Separates The Thoracic Cavity From The . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
